
Dr. Aruna Ashok MBBS, MS OG, DNB OG
- Clinical Director

Endometriosis is a chronic condition that affects millions of women worldwide. It occurs when tissue similar to the lining of the uterus, called the endometrium, grows outside the uterus.
This abnormal growth can cause various symptoms such as pelvic pain, painful periods, and infertility. One important aspect to consider when diagnosing and managing endometriosis is the thickness of the endometrial implants.
In this article, we will delve into the topic of endometriosis thickness, exploring its significance, diagnostic methods, and potential implications for treatment.
Understanding the intricacies of endometriosis thickness can help healthcare providers develop more effective strategies to alleviate symptoms and improve the quality of life for women affected by this condition.
To make things even more complicated, endometriosis thickness can vary from woman to woman — just like hairstyles, shoe sizes and the number of episodes of Grey’s Anatomy you’ve seen!
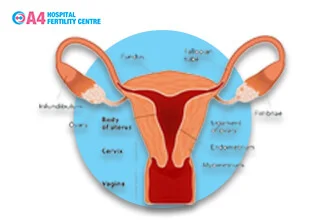
Endometriosis thickness refers to the measurement of the endometrial implants that develop outside the uterus.
These implants can vary in size, shape, and depth of infiltration into surrounding tissues.
The thickness of the endometrial tissue is an important factor in assessing the severity and extent of endometriosis.
Accurate diagnosis of endometriosis thickness is crucial for appropriate management. This is akin to a doctor needing to assess the depth of a wound before determining the appropriate treatment - the greater the depth, the more complex the treatment may be.
Transvaginal ultrasound is a commonly used imaging technique that allows visualization of the pelvic organs. It can provide valuable information about the size, location, and thickness of endometrial implants. However, this method may not be sufficient for detecting all types and locations of endometriosis lesions.
MRI is a more advanced imaging technique that can offer detailed visualization of the pelvic structures, including endometrial implants. It provides high-resolution images and can help determine the thickness, depth, and extent of the lesions. MRI is particularly useful in cases where ultrasound results are inconclusive or when deep infiltrating endometriosis is suspected.
Laparoscopy is considered the gold standard for diagnosing endometriosis. It involves the insertion of a thin, lighted tube through a small incision in the abdomen to visualize the pelvic organs directly. During laparoscopy, the thickness of endometrial implants can be assessed, and tissue samples can be obtained for histopathological examination, confirming the presence of endometriosis.
The thickness of endometrial implants holds significance in several aspects of endometriosis diagnosis and management :
The thickness of endometrial implants can indicate the severity of endometriosis. Thicker lesions often suggest a more advanced stage of the disease, with deeper infiltration into surrounding tissues. Assessing thickness helps healthcare providers determine the appropriate treatment approach, considering factors such as pain management, hormonal therapy, or surgical intervention.
Endometriosis thickness can affect fertility. Thicker lesions may cause distortion and scarring of the reproductive organs, leading to infertility or difficulties in conceiving. Understanding the thickness of endometrial implants is crucial when evaluating the potential impact on fertility and guiding fertility treatments such as in vitro fertilization (IVF) or surgical interventions to restore reproductive function.
For cases where surgical intervention is necessary, knowledge of endometriosis thickness is essential. Thicker implants may require more extensive excision or removal, and surgical planning can be tailored accordingly. Identifying the thickness of endometrial lesions also aids in determining the involvement of adjacent organs, helping surgeons anticipate challenges and optimize the surgical approach.
Treatment strategies for endometriosis aim to relieve symptoms, manage pain, and improve fertility. The choice of treatment depends on various factors, including the thickness and extent of endometrial implants :
Thicker lesions often correlate with increased pain severity. Nonsteroidal anti-inflammatory drugs (NSAIDs) and hormonal therapies, such as oral contraceptives or gonadotropin-releasing hormone (GnRH) agonists, are commonly prescribed to manage pain associated with endometriosis. In severe cases, surgery may be necessary to remove the thickened lesions and alleviate pain.
Hormonal therapies can help regulate the menstrual cycle, reduce inflammation, and suppress the growth of endometrial implants. The choice of hormonal therapy depends on various factors, including the thickness of endometrial lesions, the severity of symptoms, and the woman's reproductive goals.
In cases where conservative treatments fail or when fertility is a concern, surgical intervention may be necessary. Laparoscopic excision or ablation of endometrial implants is commonly performed. Thicker lesions may require more extensive surgical excision, while fertility-preserving techniques can be employed whenever possible.
Understanding the thickness of endometrial implants is crucial in diagnosing and managing endometriosis effectively. Diagnostic methods such as transvaginal ultrasound, MRI, and laparoscopy help assess the thickness and extent of endometriosis lesions. The thickness of endometrial implants serves as a valuable indicator of disease severity, fertility implications, and aids in surgical planning. Treatment options, including pain management, hormonal therapy, and surgical interventions, can be tailored based on the thickness of endometrial lesions. By considering endometriosis thickness, healthcare providers can offer more personalized and effective care to women affected by this challenging condition, ultimately improving their quality of life and reproductive outcomes. Of course, healthcare providers should also remember to take into account the patient's sense of humor and willingness to laugh at endometriosis-related puns!